We have selected 22 basic questions about prostatitis and its treatment. All answers are written by our leading male health specialist, andrologist. We hope that this article will help you and give you the necessary answers to your questions.
Symptoms of prostatitis: pain, burning, discharge, stinging, incontinence
Symptoms for prostatitis are most often of 3 types:
- violation of urination: difficult, frequent, nocturnal urination.
- pain symptoms: pain in the perineum, lower abdomen, groin. Pain can radiate (give) to the scrotum or sacrum.
- mixed form, in which there are both urinary disorders and pain.
What causes prostatitis?
With bacterial prostatitis
The infection enters the prostate gland from neighboring organs:
- urethra;
- Bladder
- through the blood and lymphatic vessels from a remote inflammatory focus (tonsillitis, sinusitis, caries).
The most common bacteria detected in prostatitis are: Escherichia coli, Klebsiella, Proteus, Staphylococcus aureus, Enterococcus.
The role of sexually transmitted infections is discussed: chlamydia, mycoplasma, Trichomonas.
The activity and, accordingly, the manifestation of the inflammatory process depends on the properties of the microorganism, on the condition of the pelvic organs, their blood circulation, concomitant diseases and other predisposing factors.
With non-bacterial prostatitis
Stagnation plays an important role. Violation of blood flow causes edema, exudation of prostate tissue and creates conditions for the development of an inflammatory process that is not associated with a bacterial agent.
STDs and prostatitis
The question of the involvement of sexually transmitted infections in the development of prostatitis is widely discussed in scientific medical circles. There is no consensus on this matter.
We regard ourselves as supporters of a direct connection between infections, the onset and course of prostatitis.
Why is prostatitis dangerous?
Prostatitis does not pose a threat to the patient's life, the process is chronic and worsens the quality of life.

Beginning prostatitis. How to determine? First signs
The first signs of prostatitis are changes in the nature of urination: difficult, frequent urination, frequent urge to urinate, especially at night. Discomfort during urination and pain of varying intensity in the groin area.
Age of Prostatitis? Is this a disease of the young and / or the old?
Prostatitis is an inflammatory disease, so it can occur at any age. But adenoma or hyperplasia of the prostate is an age-related disease in men after 50 years of age and is associated with the development of a benign prostate tumor.
Chronic prostatitis. Is it possible to cure?
The presence of a diagnosis of chronic prostatitis implies the presence of changes in the structure of the tissues of the gland, which remain for life. Like any chronic disease, prostatitis proceeds with alternating periods of exacerbation and remission - a period when the patient is not worried about anything. With proper treatment and lifestyle, periods of remission can be very long, and complaints never bother the patient again.
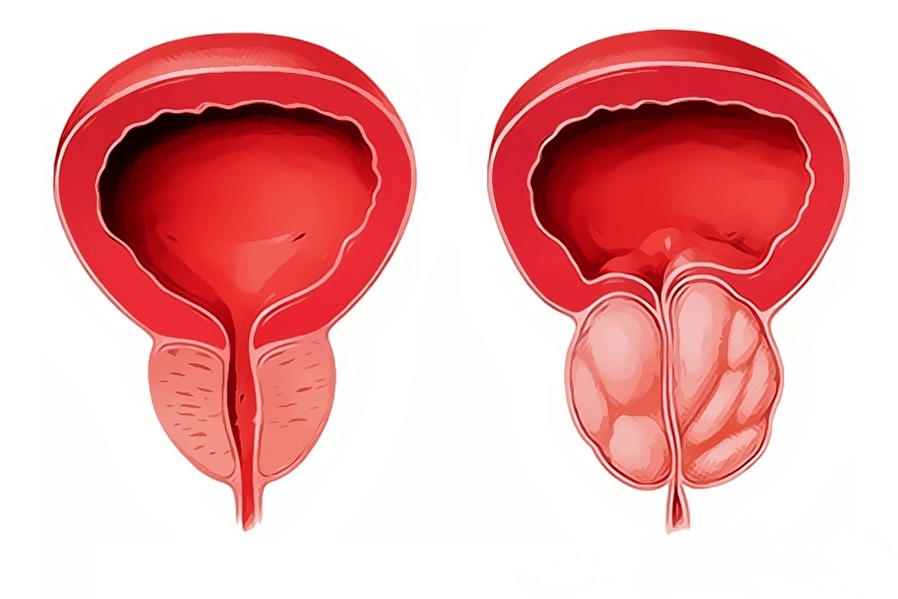
Bacterial and other types of prostatitis
There are various classifications, the most commonly used being developed by the US Institutes of Health in 1995:
- Category I.Acute prostatitis.
- Category II.Chronic bacterial prostatitis.
- Category III.Non-Bacterial Prostatitis / Chronic Pelvic Pain Syndrome - with no obvious signs of infection and lasting 3 months or more.
- Subcategory III A.Chronic inflammatory pelvic pain syndrome (with leukocytes in the secretion of the prostate and excretion of the pathogen).
- Subcategory III B.Syndrome of chronic non-inflammatory pelvic pain (no leukocytes in the secret of the prostate).
- Category IV.Asymptomatic prostatitis (with leukocytes in the secret of the prostate, but without complaints).
For ease of understanding, the classification can be presented in 3 types:
Acute prostatitis- proceeds with severe pain, fever, urinary disorders. The secret of the prostate is a large number of leukocytes, which indicates a clear inflammatory process. It occurs, as a rule, for the first time in a given patient. If these symptoms occur in a patient with chronic prostatitis, then they are referred to as an exacerbation of chronic prostatitis.
Chronic bacterial prostatitis- Symptoms that periodically disturb the patient, as a rule, are less pronounced than in acute prostatitis. When diagnosing an increase in leukocytes in the secret of the prostate, it is possible to identify the causative agent of inflammation.
The most problematic for diagnosis isnon bacterial prostatitis, or so calledchronic pelvic pain syndrome. . . This is due to the fact that the complaints are very similar to prostatitis, but associated with diseases of other organs and systems, in which it is not possible to detect signs of inflammation and pathogenic bacteria: spasm of the pelvic muscles, impaired interaction between the muscles of the bladder and its sphincter, anatomical disorders - strictures(narrowing) of the urethra, leads to inflammation due to increased pressure inside the lobules of the prostate gland.
Who treats prostatitis - andrologist or urologist?
Prostatitis is treated by both a urologist and an andrologist.
An andrologist is a urologist specializing in male reproductive and reproductive diseases.
Methods and treatment regimens for prostatitis
All treatment regimens for the prostate gland consist of drugs:
- anti-inflammatory
- antibacterial
- biogenic stimulants
- drugs that improve the contraction of the prostate and bladder while relaxing the sphincter.
Good results are obtained by the simultaneous appointment of drugs and physiotherapy (prostate massage, complexes for the treatment of prostatitis).
What tests are given for prostatitis?
Fordiagnosis of prostatitisconsultation of a urologist (andrologist) is required in order to collect patient complaints, medical history, microscopy of prostate secretions and ultrasound diagnostics.
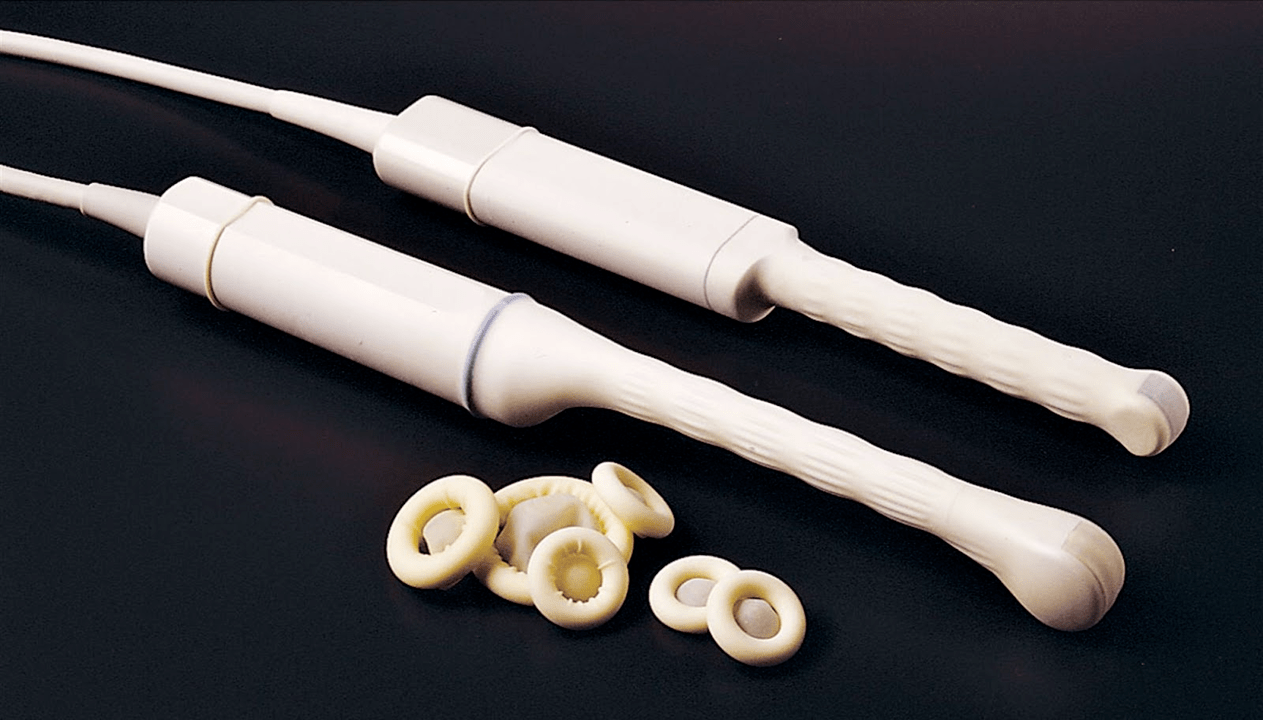
For diagnostics, transrectal ultrasound of the prostate gland (TRUS) and prostate secretions obtained after prostate massage are used for microscopic examination.
In addition, the sowing of the secretion of the prostate gland on the bacterial flora with the determination of the sensitivity of the seeded microflora to antibiotics can be used.
Surgical interventions and operations for prostatitis
With prostatitis, operations are practically not used. With the exception of prostate abscess - a process in which foci with purulent contents are formed.
Is it possible to cure prostatitis yourself?
In the presence of severe symptoms, it is better to be treated by a specialist, the time factor plays an important role in treatment, since the longer the inflammation lasts, the more likely it is that irreversible changes in the organ are.
But it is better to do prevention yourself, no doctor will do it for you.
Avoid hypothermia, congestion during prolonged sitting, sexually transmitted infections, irregular sexual activity - all this is the way to effective prevention of prostatitis.
Medicines for prostatitis: finalgon, vitaprost, prostamol, ceftriaxone, doxycycline, omnix and others
Medicines for the treatment of prostatitis are divided into groups according to the mechanism of action:
Antibacterial agents (antibiotics)are prescribed only if there is a diagnosis: chronic bacterial prostatitis. The most commonly used fluoroquinolones, macrolides and the doxycycline group of drugs.
Alpha blockers:are prescribed to restore impaired urination, increasing the contraction of the bladder and relaxing its detrusor.
Large groupbiogenic stimulants and herbal preparations: candles.
Effective treatment is possible only with the correct diagnosis, since there are no universal medicines for all types of prostatitis. Often, patients take drugs for the treatment of prostatitis, if they have a completely different disease, but with similar symptoms.

Nuts, roots, parsley, cucumber, honey, bees, leeches and other folk treatments for prostatitis
Traditional methods of treatment have a right to exist, but you need to understand that it is very difficult to choose a folk method that suits you. On request, the search engine gives out 70 million results for the treatment of prostatitis with folk methods.
Nobody has researched folk methods for effectiveness. The fact that it helped one patient with such treatment (and whether it helped) does not mean that it will help you.
Exacerbation of prostatitis after treatment. Remission, relapse
All chronic inflammatory processes have periods of exacerbation and remission, when the patient is not worried about anything. The duration of remission can vary and depends on many factors, including whether the patient is undergoing prophylactic treatment. Patients who periodically carry out preventive treatment, without waiting for a deterioration in well-being, usually have more rare exacerbations.

Massage of the prostate gland at home. Is massage always necessary for prostatitis?
Prostate massage can also be done at home if you are married to a nurse in the urology office. Any medical manipulation has its own subtleties and nuances. Only a doctor can determine the indications for this procedure, so for some diseases: prostate adenoma (in the presence of acute urinary retention), prostate massage is not desirable, and in case of tumors, it is contraindicated.

Alcohol and prostatitis
Alcohol, by itself, does not cause the development of prostatitis, but is a factor that increases the congestion and edema of the prostate gland and, thereby, contributes to its development.
Sex life and prostatitis
There is a direct link between the intensity of sexual activity and prostate disease. With prolonged abstinence in the prostate, stagnation occurs, which impairs metabolic processes, and disrupts blood microcirculation, contributing to the development of inflammatory processes. Regularity is more important to the health of the prostate gland than the intensity of sexual intercourse. Excessive sexual intercourse, especially with different partners and unprotected from infections, is the fastest way to prostatitis.

Does prostatitis affect women?
Of course, there is an effect on the health of a woman with prostatitis in a partner. The prostate, together with the seminal vesicles, produces a liquid component of the sperm, which, during intercourse, enters the partner's genital tract. The main danger may be the presence of a sexually transmitted infection or bacterial prostatitis, which can provoke inflammatory diseases in a woman.
Pregnancy and prostatitis
Since the prostate gland produces a liquid portion of sperm that contains nutrients for sperm, prostatitis often results in a decrease in sperm quality, making it difficult to get pregnant.
Prevention. What to do to avoid prostatitis?
Prevention is directly related to the patient's climate and profession.
Prevention of prostatitis is about avoiding and minimizing the factors that contribute to the development of prostatitis. It is necessary to avoid hypothermia, alternate sedentary work with periods of physical activity. Regular sex life is important for prostatitis.























