Prostatitis in women is not a joke, but a colloquial name for inflammation of the vestibule glands. These glands are also called Skene's glands, and their inflammation - skinitis - manifests the same symptoms as prostatitis in men. What are the features and danger of this disease?
Does prostatitis happen in women?

The insidiousness of pathology is that it is poorly detected by doctors and is rare.
Prostatitis in women does happen, but the disease is called skinitis. The glands that become inflamed in this pathology are located slightly below the urethra and are composed of sensitive tissue.
The Skene's glands are thought to be a rudimentary prostate that forms in the embryo before the genitals appear. Simply put, Skene's glands are a kind of blank that develops into a full-fledged prostate gland in a male fetus, and remains in its infancy in a female fetus.
It is interesting that these glands are capable of producing a specific secretion, which is identical in composition to the secretion of the prostate gland in men. Moreover, the PSA antigen, which is the most important tumor marker, can be found in this fluid.
Interesting!The jet orgasm that occurs in some women is the result of the activity of Skene's glands.
Skineitis is rare. The problem is that female prostatitis is difficult to diagnose, often misdiagnosed, so there are no accurate statistics on the prevalence of this disease.
Reasons for the development of skinite
Most women are not even aware of the presence of these glands near the urethra, but when they become inflamed, acute symptoms appear, reminiscent of the signs of prostatitis in men.
Skinitis is most often caused by an infection of the glands. The main reasons for the development of the disease:
- damage to the urethra;
- lack of hygiene;
- infection of the glands due to the spread of infection in other diseases of the genital organs.
Most often, skinitis is caused by opportunistic microorganisms that inhabit the female body. They can enter the glands in the urine during urination, or from the vagina. Under normal conditions, such microorganisms do not cause an inflammatory process, however, when Skene's glands or urethra are injured, female prostatitis occurs. This is due to a decrease in local immunity.
Skineitis can be of an allergic nature. The use of substandard intimate hygiene products can cause an allergic reaction and a decrease in local immunity, as a result of which the risk of infection of the glands increases.
Another reason for the development of skinitis in women is trauma to the urethra due to surgery or rough intercourse. It is also possible to damage the opening of the urethra due to urolithiasis, when sand passes through the urethra.
"Prostatitis" in a woman is associated with an irregular sex life. Frequent change of sexual partners and neglect of barrier contraception increases the risk of developing urogenital infections.
A factor that increases the risk of developing this disease is a general decrease in immunity. Skineitis can be associated with recent severe infectious diseases, hypothermia, exacerbation of chronic diseases.
Symptoms of the disease

With pathology, constant weakness and "weakness" is felt throughout the body.
Having figured out whether a woman has prostatitis, you should know how skinitis manifests itself. The disease is called "female prostatitis" largely due to symptoms that resemble inflammation of the prostate in men. When discarding, the symptoms are as follows:
- frequent urge to urinate;
- urination in small portions;
- pain and pain in the urethra when using the toilet;
- soreness during intercourse;
- increased body temperature;
- spasms in the bladder area;
- general malaise, loss of strength.
Skineitis in many ways resembles cystitis in women. With this disease, the urge to urinate is constantly felt, but this need cannot be fully satisfied. Urine is excreted in small portions, and this is accompanied by severe discomfort. The feeling of full bladder persists even when using the bathroom.
You can distinguish skinitis from other diseases of the genitourinary system with similar symptoms by the presence of pain during intercourse.
There is no intense heat with skinite, but the body temperature can rise to 37. 5-38 degrees.
Why is prostatitis in women dangerous?
Having understood the peculiarities of this disease, the patients ask the question of whether such prostatitis is dangerous for women. This disease can lead to dangerous complications, therefore, requires timely diagnosis and treatment.
Among the probable complications of skinitis:
- abscess of the gland;
- cystic neoplasms;
- secondary infertility;
- adhesions in the small pelvis;
- deformation of the area where the inflamed glands are located;
- spread of infection to other organs of the small pelvis.
The disease is infectious and can be caused by pyogenic bacteria. In severe cases, inflammation can develop into a glandular abscess, which is accompanied by severe symptoms and requires surgical treatment. An independent breakthrough of an abscess is potentially dangerous with the development of sepsis (blood poisoning).
The infection can spread through the bloodstream to all organs of the small pelvis. There is also a risk of upward spread of disease-causing agents with subsequent kidney infection. In addition, with extensive infection, a woman can infect a partner through unprotected intercourse. In men, bacterial urethritis can develop into prostatitis.
Diagnostics
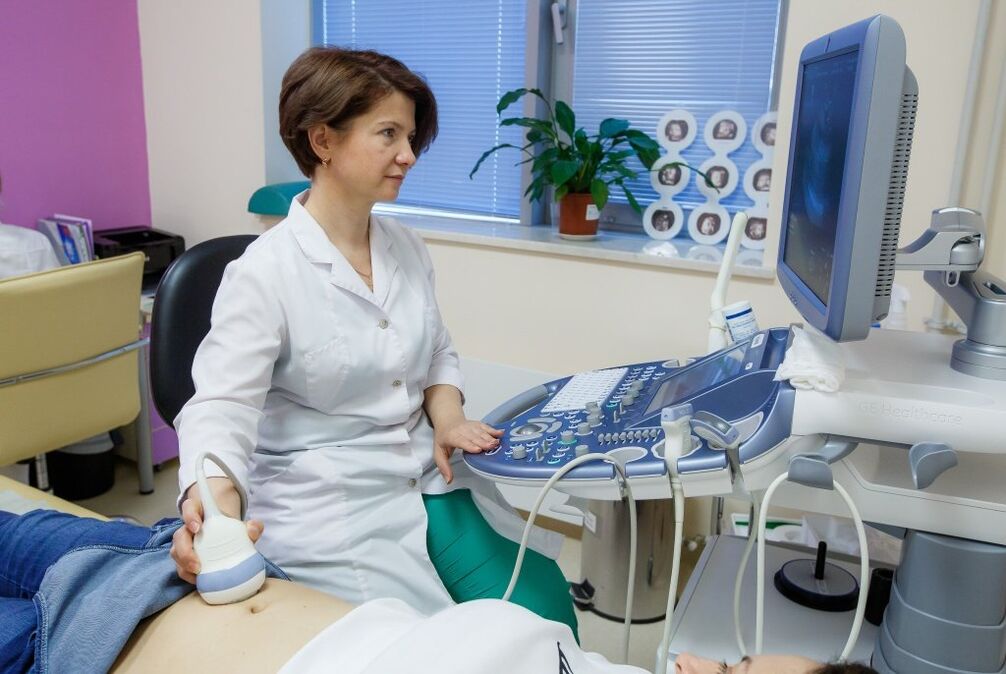
Ultrasound diagnostics are performed to make sure that there are no other diseases.
Having figured out whether prostatitis exists in women and by what signs and symptoms one can suspect skinitis, it is recommended not to self-medicate, but to immediately seek medical help.
The main problem with skinitis is complex diagnostics. Due to the specifics of the location of the glands, their inflammation is accompanied by symptoms of inflammation of the bladder or urethral mucosa, therefore, the wrong diagnosis is often made and the wrong treatment regimen is prescribed.
Skene's gland is located in a hard-to-reach place, so it is impossible to fully examine it. In this regard, the diagnosis is made by excluding other diseases with similar symptoms. Required examinations:
- Ultrasound of the bladder to exclude cystitis;
- Ultrasound of the uterus and appendages to exclude inflammation;
- smear from the cervical canal;
- bacterial culture from the cervix;
- general and biochemical urine analysis;
- a smear from the urethra.
After the exclusion of other diseases, the treatment of skinitis is prescribed. Often the most informative diagnostic method is urinalysis, which detects pathogenic microorganisms.
Treatment features
With skinning, conservative treatment is practiced. Therapy includes taking drugs of the following groups:
- antibiotics to clear up the infection;
- anti-inflammatory drugs used in urology;
- antispasmodics to reduce pain;
- immunomodulators.
Usually, broad-spectrum antibiotics are prescribed, or antibacterial drugs used in the treatment of cystitis. Since it is often impossible to accurately determine the causative agent of the disease, the doctor may prescribe several drugs of this group at once. Cephalosporins of the third generation have proven themselves well.
Acute symptoms recede a day after the start of antibiotic treatment. However, it is important to take the drugs in a course, the duration of which is set by the doctor on an individual basis.
To eliminate pain, it is recommended to use antispasmodics. Simple analgesics are ineffective because pain is associated with spasm of the urethra and bladder.
Additionally, herbal anti-inflammatory drugs are prescribed, used in the treatment of cystitis and kidney disease. These drugs reduce the inflammatory process, normalize the urination process and facilitate overall well-being in various diseases of the urinary tract.
Immunomodulators are required. They use both drugs for the prevention of diseases of the genitourinary system, and fortifying agents, for example, echinacea purpurea extract.
Preventive measures
Having figured out how to cure skinitis, you should pay attention to important preventive measures. This disease is similar to cystitis - once you get sick, the chance of relapse remains for many years. To prevent this, you must:
- observe personal hygiene;
- use barrier methods of contraception;
- have a permanent sexual partner;
- strengthen immunity.
When the first alarming symptoms appear, you must immediately make an appointment with a gynecologist and urologist. Self-medication for skinitis is dangerous with chronic inflammation.























