Chronic prostatitis is a prolonged inflammation of the prostate gland, leading to impaired morphology and functioning of the prostate. Chronic prostatitis is manifested prostatic triad of pain in the pelvic region and genitals, urinary disorders, sexual disorders. Diagnosis of chronic prostatitis includes palpation of the gland, study of prostate secretion, ultrasonography, uroflowmetry, in, needle biopsy of the prostate. In chronic prostatitis shows complex medical, physiotherapy, massage prostate, instillation posterior urethra. Surgical treatment is advisable in complicated forms of chronic prostatitis.
Chronic prostatitis
Chronic prostatitis is the most common male disease: about 50% of men suffer some form of inflammation of the prostate. Chronic prostatitis often affects men aged 20 to 40 years, in the period of maximum sexual and reproductive activity. In this regard, detection and treatment of chronic prostatitis in urology is becoming not only medical but also social aspect.
Classification of chronic prostatitis
According to the modern classification of prostatitis developed in 1995, we distinguish 3 categories of disease:
- I. Acute prostatitis.
- II. Chronic prostatitis of bacterial origin.
- III. Chronic nonbacterial prostatitis Genesis/chronic pelvic pain Syndrome – a syndrome that is not associated with obvious signs of infection and continued 3 months or more.
- III A chronic prostatitis with an inflammatory component (detection in the prostate secretion white blood cells and infectious agents);
- III B chronic prostatitis with no inflammatory component (leukocytes and pathogens in the prostate secretion).
- IV. Asymptomatic chronic prostatitis (no complaints in the identification of leukocytes in prostatic secret).
In the presence of the infectious component talking about bacterial (infection) chronic prostatitis; in the absence of microbial pathogens – nonbacterial (non-contagione) prostatitis. It is believed that 90-95% of all cases there is a non-bacterial chronic prostatitis and only 10-5% is bacterial.
The causes of chronic prostatitis
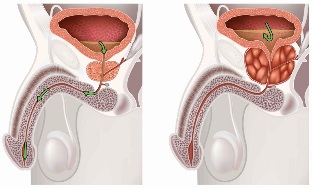
The etiology and pathogenesis of chronic bacterial prostatitis are associated with any infection in the prostate following ways: upward (through the urethra), downward (when reflux of infected urine from the bladder), hematogenous (blood highways) or lymphogenous (for lymphatic collectors). Most uropathogens are E. coli, Klebsiella, Proteus, Staphylococcus, Enterococcus, CORINE, fungal, parasitic and viral pathogens. Along with the non-specific flora the development of chronic prostatitis can take part agents specific urethritis (chlamydia, Mycoplasma, gonococcus, Trichomonas, Gardnerella).
However, for the development of chronic prostatitis it is not so much the presence and activity of micro-organisms as the state of the pelvic organs and circulation in them, the presence of comorbidities, the level of protective mechanisms.
Therefore, the emergence of chronic prostatitis can contribute to a number of factors. First of all, it urological diseases, pyelonephritis, cystitis, urethritis, stricture of the urethra, increatos until the end of acute prostatitis, orchitis, epididymitis etc. Microbial etiologist can get into the prostate from distant foci of infection, for example, sinusitis, tonsillitis, dental caries, chronic bronchitis, pneumonia, pyoderma, etc. Predispose to chronic inflammation, local and General hypothermia, overheating, stay in a humid environment, fatigue, malnutrition, rare urination, etc.
Chronic non-bacterial prostatitis is usually associated with congestive (congestive) phenomena in the prostate caused by stasis of the venous circulation in the pelvic organs and impaired drainage acini of the prostate. Local obstructio causes overflow of blood vessels of the prostate with blood, swelling of incomplete emptying of secretions, breach the barrier, secretory, motor, contractile function of the gland.
Congestive changes generally caused by behavioral factors, long-term sexual deprivation, practice, interrupted or prolonged sexual activity, excessive sexual activity, lack of exercise, prolonged sitting, chronic intoxication (alcohol, nicotine, drugs), occupational hazard (vibration). To the development of nonbacterial chronic prostatitis predisposing pathology of the pelvic organs and nerve structures of their innervation (e.g., spinal cord injury), adenoma of the prostate, hemorrhoids, constipation, androgenodeficiency, etc. reasons.
The symptoms of chronic prostatitis
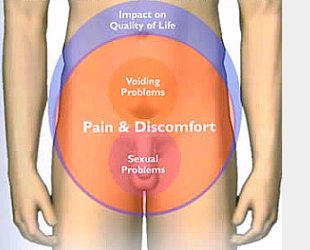
Chronic prostatitis is manifested by local and General symptoms. Local manifestations belongs prostatic triad, characterized by pain, dysuria and sexual dysfunction. Pain in chronic prostatitis are of a constant aching in nature, localized in the perineum, genitals, suprapubic, groin. Pain syndrome increases at the beginning and end of urination, with pain radiating to the glans penis, the scrotum, sacrum, the rectum. Pain may increase after sexual intercourse or in connection with long-term abstinence; to weaken or strengthen after orgasm to become more intense at the moment of ejaculation.
The intensity of the pain syndrome in chronic prostatitis varies from discomfort to Express that violate the sleep and performance manifestations. Pain with restricted localization in the sacrum are often regarded as low back pain or sciatica, in connection with a patient long treated without a physician's assistance.
Urination in chronic prostatitis and painful learning. While there may be a difficulty beginning miscet, a weakening or discontinuity of the urine stream, feeling of incomplete emptying of the bladder, frequent night urination, burning in urethra. In the urine in chronic prostatitis can detect the presence of floating threads. After a bowel movement or physical exertion of urethral appear allocation , due to a reduction in tone of the prostate. In chronic prostatitis may be a cause itching, feeling cold or excessive sweating in the crotch, a local discoloration of the skin, associated with stagnation of blood circulation.
Chronic prostatitis accompanied by severe disorders of sexual function. Phenomena gipotenzia may be worsening, painful erection, prolonged and frequent night erections, difficulty or early ejaculation, loss of libido (reduced libido), erased orgasms Hematospermias, infertility. Sexual dysfunction is always hard experienced man, leading to psycho-emotional disorders, up to neurosis and depression, even more worsen sexual function.
Exacerbation of chronic prostatitis accompanied by a slight increase in body temperature and deterioration of health. Overall condition in chronic prostatitis is characterized by increased irritability, lethargy, anxiety, fatigue, loss of appetite, sleep disturbance, reduced work capacity, creative and physical activity.
Almost a quarter of patients with chronic prostatitis symptoms for a long time absent, resulting in late treatment to the urologist. Long duration of chronic prostatitis may be complicated by impotence, vesiculitis, epididymoorchitis, male infertility, incontinence, stone formation, cysts of the prostate gland, sclerosis of the prostate, development of adenoma and prostate cancer.
Diagnosis of chronic prostatitis
Necessary for the diagnosis of chronic prostatitis information is obtained through comprehensive laboratory and instrumental examination. Initial examination for suspected chronic prostatitis include the clarification of anamnesis and complaints, conducting external inspection of the genitalia for discharge, lesions, irritations, digital rectal examination of the prostate with the aim of determining the shape, boundaries, consistency, tenderness of the breast.
To determine the structural and functional changes of the prostate is shown holding ultrasound of the prostate (TRUS). Important methods in the diagnosis of chronic prostatitis are the study of the secret prostate, urinalysis, bacteriological examination of smear from the urethra and urine, 3 cups of urine samples, PCR and REEF study scraping on pathogens of genital infections, determination of prostate-specific antigen (PSA).
Clinically significant chronic prostatitis is the detection in the analysis of causative agents of chlamydiosis, mycoplasmosis, herpes, cytomegalovirus, trichomoniasis, gonorrhea, candidiasis, and nonspecific bacterial flora. The fence prostate secretion to studies conducted after urination and massage the prostate. Symptoms of chronic prostatitis are increasing in the number of cells in field of view, reducing the number of lecithin granules, the presence of pathogenic microorganisms.
In General urine analysis in chronic prostatitis may show pyuria, pyuria, erythrocyturia. Bacteriological urine culture helps to identify the degree and nature of bacteriuria. With reproductive disorders shows a study of sperm and MAR test.
The degree and causes voiding help to determine urodynamic studies (uroflowmetry, cystometry, profilometry, electromyography). Using data from studies of chronic prostatitis could be differentiated from stress incontinence, neurogenic bladder, etc. When hematuria, Hematospermias, obstructive voiding an endoscopic examination urethroscopy, and cystoscopy. To eliminate the adenoma and prostate cancer requires the determination of PSA, in some cases, a biopsy of the prostate with the morphological study of tissues.
Treatment of chronic prostatitis
Chronic prostatitis cure difficult, but remember that recovery is still possible and largely depends on the mood of the patient, the timeliness of his appeal to the specialist for adherence to all requirements of the urologist. The mainstay of treatment of chronic bacterial prostatitis antimicrobial therapy is in accordance with antibiotics at least 2 weeks. To reduce pain and inflammation NSAIDs are appointed ; to relax the muscles of the prostate, the restoration of urodynamics and outflow prostatic secretion shows reception a-adrenoblokatorov.
With the aim of improving drainage of the prostate, local microcirculation and muscle tone is held a course of therapeutic massage the prostate. A massage of the prostate gland should result in the allocation of not less than 4 drops of prostate secretion. Prostate massage is contraindicated in acute bacterial prostatitis, abscess of the prostate, hemorrhoids, stones of the prostate, rectal fissures, hyperplasia and prostate cancer.
To relieve the pain syndrome in chronic prostatitis can be recommended paraprostatic blockade, acupuncture. Important in the treatment of chronic prostatitis plays a physiotherapy appointment of medicinal electrophoresis, ultrasound, phonophoresis, magnetic therapy, laser magneticam illic, inductometer, mud therapy, SMT, hot hip bath temperature 40 – 45°C, enemas with hydrogen sulfide and mineral waters, instillation into the urethra.
With the development of complications associated with chronic prostatitis surgical treatment: the removal of strictures of the urethra; TUR of the prostate or prostatectomy when sclerosis prostate; transurethral resection of the bladder with multiple sclerosis his neck, puncture and drainage of cysts and abscesses of the prostate; circumcisio with phimosis caused by recurrent urinary tract infections, etc.
Prevention of chronic prostatitis
Prevention of chronic prostatitis requires compliance with genital hygiene, timely treatment of urogenital and extragenital infections, normalization of regularity sexual life, sufficient physical activity, prevent constipation, timely emptying of the bladder.
To avoid recurrences of chronic prostatitis necessary dynamic checks andrologist (urologist); preventive courses of physiotherapy, multivitamins, immunomodulators, with the exception of hypothermia, overheating, stress, bad habits.























